Introduction
 Zoanthids have been a popular choice in the aquarium industry due to their bright colors, and ease of care for many years. Recent stories in both online forums and major news feeds have brought these brightly colored corals back into the spotlight with a negative tint. But what exactly is palytoxin, and how does it work? What signs should I be aware of with possible exposure?
Zoanthids have been a popular choice in the aquarium industry due to their bright colors, and ease of care for many years. Recent stories in both online forums and major news feeds have brought these brightly colored corals back into the spotlight with a negative tint. But what exactly is palytoxin, and how does it work? What signs should I be aware of with possible exposure?
The History
 Palytoxin was first described in the literature by Moore and Scheuer in 1971. This initial description recounted an ancient Hawaiian legend called “Limu Make o Hana”, which translates to “deadly seaweed of Hana”. Warriors would inoculate their spear points with the seaweed from a specific pool to make the their wounds fatal. Research by Walsh and Bowers described this ancient pool as not containing seaweed, but rather an undescribed species of zoanthid, Palythoa toxica. It was not until almost a decade later that the structure of palytoxin was revealed by Dr. Hirata and Dr. Moore independently.
Palytoxin was first described in the literature by Moore and Scheuer in 1971. This initial description recounted an ancient Hawaiian legend called “Limu Make o Hana”, which translates to “deadly seaweed of Hana”. Warriors would inoculate their spear points with the seaweed from a specific pool to make the their wounds fatal. Research by Walsh and Bowers described this ancient pool as not containing seaweed, but rather an undescribed species of zoanthid, Palythoa toxica. It was not until almost a decade later that the structure of palytoxin was revealed by Dr. Hirata and Dr. Moore independently.
The Toxin
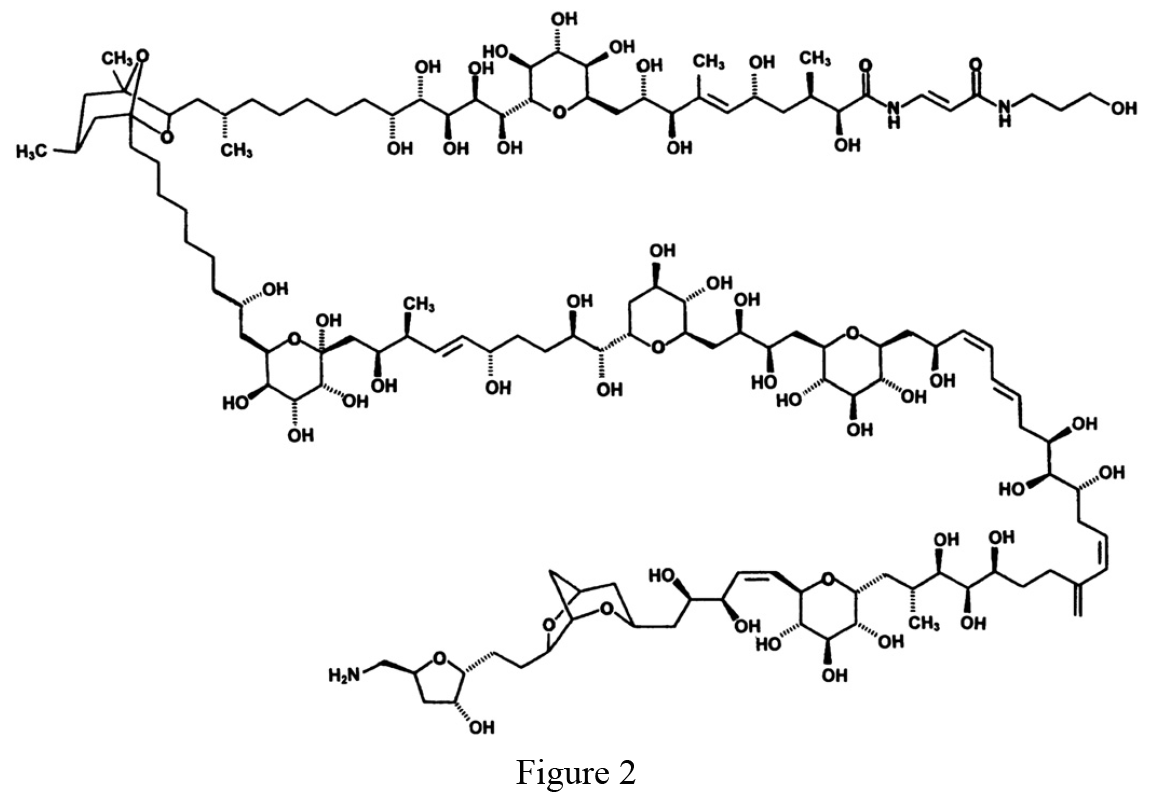
From the initial collection of Palythoa toxica a non-protein compound was collected. This work was done by Dr. Friedrich Hoffman on the original samples collected by Moore and Scheuer. This compound had a molecular weight of 2680.17 g/mol (1), with a LD50 (lethal dose of 50% of test subjects) of between 0.03 and 0.45 micrograms/kg (3). In humans, the LD50 dose is between 2.3 and 31.5 micrograms (3). This makes palytoxin one of the most toxic non-protein substances known to date. Palytoxin has the molecular structure of C129H223N3O54, shown in figure 2. The molecule exists as a dimer in aqueous solutions (3). The molecule contains a large aliphatic backbone, and is both lipophilic and hydrophilic. Variation of the molecular structure of palytoxin does exist in nature with 8 variations currently described in the literature.
Palytoxin is not limited to palyanthids and zoanthids. It has been isolated from red algae, anemone, sea urchins, polychaete worm, and multiple dinoflagellate species (2). It has also been documented within the reef associated food web including many fish species and crabs containing the toxin. Palytoxin has been implicated in human illness following consumption of parrotfish, groupers, smoked fish, sardines, and crab (3).
The initial work on the toxicity of palytoxin was conducted at the US Army Toxicology Division in Maryland (2). Studies were conducted with various lab animals on the toxicity of palytoxin on multiple modes of transmission. Exposures tested included intramuscular, subcutaneous, intraperitoneal, intra tracheal, intragastric, intrarectal, percutaneous, and ocular (2). The lethal doses or LD50 were reported for each animal species and exposure method at 24 hours. Of all the animal models, intravenous exposure showed the greatest toxicity. Intramuscular injections showed a 2.5 fold increase in the lethal dose in dogs and rats compared to intravenous injections (2).
Symptoms of the toxin were described for all the animal models individually in these studies. Primate models showed ataxia or loss of control of movements, drowsiness, limb weakness, and vomiting in some animals. Histological review of the animals showed damage to multiple organs including the liver, lungs, kidneys, brain, and gastrointestinal tract (2).
Pharmacology: How does Palytoxin work?
Palytoxin has been shown to attack every animal cell type it has been studied in, causing a wide range of symptoms and effects (3). It has been shown to cause very strong contractions in all muscles types including cardiac muscle, cause increased secretions by secretory cells, and depolarize other cells (3).
Palytoxin works as an irreversible antagonist of the sodium-potassium ATPase effectively permanently turning it off. The toxin also causes a change in the conformation or shape of the ATPase turning it into an open channel. This allows sodium, and other cations (positively charged molecules) to move into the cell, and cause a depolarization event. Along with sodium, calcium, and hydrogen ions are allowed to pass into the cell. In red blood cells palytoxin has been shown to hindered carbon dioxide transport in the body, and a metabolic acidosis or acidification of the blood occurs. Acidification also occurs in the red blood cells and eventually leads to lysis or death of the cells.
In cardiac tissues this increased influx of calcium causes an increase in the contractility of cardiac myocytes, and increased oxygen demand of the muscle.
Clinical Manifestations
Symptoms associated with toxicity from palytoxin vary widely, and greatly depend on the route of exposure to the toxin. It is important to also keep in mind that these symptoms are the result of case files, or reports of symptoms given by those exposed collected over time.
Ingestion of the toxin is the only route of exposure that has been reported in mortalities in humans (3).
One of the most commonly reported symptoms of palytoxin exposure is rhabdomyolysis. This was seen with toxin gaining access to the circulation. Rhabdomyolysis is a disorder characterized by muscle pain, and weakness. It can also be accompanied by vomiting and confusion. Rhabdomyolysis occurs due to damage to skeletal muscle, and resulting leakage of myoglobin into circulation. Myoglobin is eventually filtered out in the urine resulting in a brown or “tea” colored urine. Large quantities of myoglobin can lead to kidney injury or even kidney failure.
Cardiac symptoms are also commonly reported following exposure. Tachycardia or heart rate over 100 beats per minute, chest pain ,and hypertension have been reported. More serious cardiac manifestations including echocardiogram abnormalities have also been reported, but not as common (see case report below). It is unknown currently the long term damage caused by palytoxin on cardiomyocytes.
Inhalation exposure to palytoxin produces its own set of symptoms upon exposure. Rhinorrhea (runny nose), cough, mild dyspnea or shortness of breath, bronchoconstriction, and fever have all been reported.
Dermal or skin contact to palytoxin was described by Hoffmann et al. in 2008 from data collected from Germany. In this case report a man collapsed approximately 16 hours after receiving multiple cuts while handling zoanthids in a home aquarium. His initial symptoms were reported 2 hours after contact. These included shivering, myalgia or muscle pain, and a generalized weakness to his extremities. His symptoms progressed to dizziness and his speech was affected prior to his collapse. At the site of his cutes, edema or swelling was noted. Examination at the hospital revealed electrocardiogram abnormalities, most notable was a right bundle branch block with a widened QRS complex (2).
Treatment
Currently no anti-toxin exists for palytoxin. Supportive measures and intravenous fluids are the mainstays of treatment currently. Patients with suspected palytoxin need close monitoring in an intensive care unit to watch for the possible cardiac and renal issues that can occur. While that may seem scary to many of you reading this, this has proven successful in managing the illness from exposure to palytoxin if initiated timely. In the case reported above from Germany the individual recovered. His electrocardiogram and cardiac function returned to normal within 24 hours after fluids were administered. IV fluids are also the mainstay of treatment for rhabdomyolysis.
How to protect yourself?
The first step in protecting yourself from palytoxin is being aware of its existence, and practice safe aquarium habits. This includes wearing eye protection and gloves while handling anything in your aquarium and during cleanings. Having aquariums in well ventilated rooms will also greatly reduce the risk of inhalation exposures. I have seen many images of fish rooms and fragging setups in closets, and areas without proper ventilation.
Leave fragging to the professionals! I have been guilty of this one myself many times, and conducted a lot of research in how to safely frag zoanthids. Personally, I wear a medical grade respirator, chemistry quality eye protection, and heavy duty gloves when handling zoanthids for fragging. I also conduct the fragging outside when possible to help reduce the risk of air borne toxin.
Another import thing to keep in mind is how to deal with rocks in an aquarium. Many people will attempt to clean rocks with hot water, or boiling techniques. This will cause the toxin to become aerosolized, and inhalation is one of the major routes of exposure in the aquarium industry. Even though you can not see zoas, does not mean some may be hiding! Acid baths outside have been effective at cleaning rocks while neutralizing the toxin, and just purchasing new rocks may be the safest.
If you have experienced any of the symptoms described after working with your aquarium do not hesitate in contacting your local health care provider.

Image from Chau H. Wu, 2009.
I am currently working on a wallet card to keep on hand to provide to medical providers in the event of a possible palytoxin exposure. Look for future posting here to download your Palytoxin Card!!!
Sources:
1. National Center for Biotechnology Information. PubChem Compound Database; CID=11105289, https://pubchem.ncbi.nlm.nih.gov/compound/11105289 (accessed May 5, 2017).
2. Jonathan R. Deeds, Michael D. Schwartz. Human risk associated with palytoxin exposure. Toxicon. 2010, Vol.56: 150-162.
3. Pilar Riobo, Jose M. Franco. Palytoxins: Biological and chemical determination. Toxicon. 2011, Vol.57: 368-365.
4. Chau H. Wu. Palytoxin: Membrane mechanisms of action. Toxicon. 2009, Vol.54: 1183-1189.
The History
The Toxin
From the initial collection of Palythoa toxica a non-protein compound was collected. This work was done by Dr. Friedrich Hoffman on the original samples collected by Moore and Scheuer. This compound had a molecular weight of 2680.17 g/mol (1), with a LD50 (lethal dose of 50% of test subjects) of between 0.03 and 0.45 micrograms/kg (3). In humans, the LD50 dose is between 2.3 and 31.5 micrograms (3). This makes palytoxin one of the most toxic non-protein substances known to date. Palytoxin has the molecular structure of C129H223N3O54, shown in figure 2. The molecule exists as a dimer in aqueous solutions (3). The molecule contains a large aliphatic backbone, and is both lipophilic and hydrophilic. Variation of the molecular structure of palytoxin does exist in nature with 8 variations currently described in the literature.
The initial work on the toxicity of palytoxin was conducted at the US Army Toxicology Division in Maryland (2). Studies were conducted with various lab animals on the toxicity of palytoxin on multiple modes of transmission. Exposures tested included intramuscular, subcutaneous, intraperitoneal, intra tracheal, intragastric, intrarectal, percutaneous, and ocular (2). The lethal doses or LD50 were reported for each animal species and exposure method at 24 hours. Of all the animal models, intravenous exposure showed the greatest toxicity. Intramuscular injections showed a 2.5 fold increase in the lethal dose in dogs and rats compared to intravenous injections (2).
Symptoms of the toxin were described for all the animal models individually in these studies. Primate models showed ataxia or loss of control of movements, drowsiness, limb weakness, and vomiting in some animals. Histological review of the animals showed damage to multiple organs including the liver, lungs, kidneys, brain, and gastrointestinal tract (2).
Pharmacology: How does Palytoxin work?
Palytoxin has been shown to attack every animal cell type it has been studied in, causing a wide range of symptoms and effects (3). It has been shown to cause very strong contractions in all muscles types including cardiac muscle, cause increased secretions by secretory cells, and depolarize other cells (3).
Palytoxin works as an irreversible antagonist of the sodium-potassium ATPase effectively permanently turning it off. The toxin also causes a change in the conformation or shape of the ATPase turning it into an open channel. This allows sodium, and other cations (positively charged molecules) to move into the cell, and cause a depolarization event. Along with sodium, calcium, and hydrogen ions are allowed to pass into the cell. In red blood cells palytoxin has been shown to hindered carbon dioxide transport in the body, and a metabolic acidosis or acidification of the blood occurs. Acidification also occurs in the red blood cells and eventually leads to lysis or death of the cells.
In cardiac tissues this increased influx of calcium causes an increase in the contractility of cardiac myocytes, and increased oxygen demand of the muscle.
Clinical Manifestations
Symptoms associated with toxicity from palytoxin vary widely, and greatly depend on the route of exposure to the toxin. It is important to also keep in mind that these symptoms are the result of case files, or reports of symptoms given by those exposed collected over time.
Ingestion of the toxin is the only route of exposure that has been reported in mortalities in humans (3).
One of the most commonly reported symptoms of palytoxin exposure is rhabdomyolysis. This was seen with toxin gaining access to the circulation. Rhabdomyolysis is a disorder characterized by muscle pain, and weakness. It can also be accompanied by vomiting and confusion. Rhabdomyolysis occurs due to damage to skeletal muscle, and resulting leakage of myoglobin into circulation. Myoglobin is eventually filtered out in the urine resulting in a brown or “tea” colored urine. Large quantities of myoglobin can lead to kidney injury or even kidney failure.
Cardiac symptoms are also commonly reported following exposure. Tachycardia or heart rate over 100 beats per minute, chest pain ,and hypertension have been reported. More serious cardiac manifestations including echocardiogram abnormalities have also been reported, but not as common (see case report below). It is unknown currently the long term damage caused by palytoxin on cardiomyocytes.
Inhalation exposure to palytoxin produces its own set of symptoms upon exposure. Rhinorrhea (runny nose), cough, mild dyspnea or shortness of breath, bronchoconstriction, and fever have all been reported.
Dermal or skin contact to palytoxin was described by Hoffmann et al. in 2008 from data collected from Germany. In this case report a man collapsed approximately 16 hours after receiving multiple cuts while handling zoanthids in a home aquarium. His initial symptoms were reported 2 hours after contact. These included shivering, myalgia or muscle pain, and a generalized weakness to his extremities. His symptoms progressed to dizziness and his speech was affected prior to his collapse. At the site of his cutes, edema or swelling was noted. Examination at the hospital revealed electrocardiogram abnormalities, most notable was a right bundle branch block with a widened QRS complex (2).
Treatment
Currently no anti-toxin exists for palytoxin. Supportive measures and intravenous fluids are the mainstays of treatment currently. Patients with suspected palytoxin need close monitoring in an intensive care unit to watch for the possible cardiac and renal issues that can occur. While that may seem scary to many of you reading this, this has proven successful in managing the illness from exposure to palytoxin if initiated timely. In the case reported above from Germany the individual recovered. His electrocardiogram and cardiac function returned to normal within 24 hours after fluids were administered. IV fluids are also the mainstay of treatment for rhabdomyolysis.
How to protect yourself?
The first step in protecting yourself from palytoxin is being aware of its existence, and practice safe aquarium habits. This includes wearing eye protection and gloves while handling anything in your aquarium and during cleanings. Having aquariums in well ventilated rooms will also greatly reduce the risk of inhalation exposures. I have seen many images of fish rooms and fragging setups in closets, and areas without proper ventilation.
Leave fragging to the professionals! I have been guilty of this one myself many times, and conducted a lot of research in how to safely frag zoanthids. Personally, I wear a medical grade respirator, chemistry quality eye protection, and heavy duty gloves when handling zoanthids for fragging. I also conduct the fragging outside when possible to help reduce the risk of air borne toxin.
Another import thing to keep in mind is how to deal with rocks in an aquarium. Many people will attempt to clean rocks with hot water, or boiling techniques. This will cause the toxin to become aerosolized, and inhalation is one of the major routes of exposure in the aquarium industry. Even though you can not see zoas, does not mean some may be hiding! Acid baths outside have been effective at cleaning rocks while neutralizing the toxin, and just purchasing new rocks may be the safest.
If you have experienced any of the symptoms described after working with your aquarium do not hesitate in contacting your local health care provider.
Image from Chau H. Wu, 2009.
I am currently working on a wallet card to keep on hand to provide to medical providers in the event of a possible palytoxin exposure. Look for future posting here to download your Palytoxin Card!!!
Sources:
1. National Center for Biotechnology Information. PubChem Compound Database; CID=11105289, https://pubchem.ncbi.nlm.nih.gov/compound/11105289 (accessed May 5, 2017).
2. Jonathan R. Deeds, Michael D. Schwartz. Human risk associated with palytoxin exposure. Toxicon. 2010, Vol.56: 150-162.
3. Pilar Riobo, Jose M. Franco. Palytoxins: Biological and chemical determination. Toxicon. 2011, Vol.57: 368-365.
4. Chau H. Wu. Palytoxin: Membrane mechanisms of action. Toxicon. 2009, Vol.54: 1183-1189.












